It’s been so long since I’ve written one of these, I don’t even know where to start. If you followed my posts during pregnancy, you may recall my struggle with SPD. Around 36 weeks, I used my walker to get to the laundry room, and I tripped over a shoe. My right foot went forward about 3 feet and I landed hard on it, with my legs apart. SNAP! That’s literally all it took to tear my SP joint (symphysis pubis). I screamed so loudly that Milkman and all 3 kids came running in. Milkman had to help drag me to the couch where I sat wailing with an ice pack. I was so angry at my body, that had been so much stronger this time, and so well supported by the HG harness (of course, I wasn’t wearing it when I tripped ::face palm::), that it just seemed cruel to make it so far and then have such a catastrophic injury at the end.
I went to the perinatologist a few days later who confirmed the tear, and later that day a wheelchair was delivered to my front door step. I was both relieved to have a means to get around, and then discouraged to know I was ending another pregnancy in a wheelchair.

The last few weeks of my pregnancy were spent sitting in the nursing chair in the corner of my livingroom, relying on my children to keep themselves fed with easy meals, and folding laundry and baby clothes while I cried missing our foster baby who had left unexpectedly the previous month. The pain I was in was unbelievable. Even readjusting myself in the recliner was scream-worthy. The last 2 weeks of my pregnancy, my mom and sisters took turns showing up most days of the week. My oldest sister swept and mopped my floors, my middle sister tended to kids, and my mother kept us all fed. This was the most help I had ever received during a pregnancy, and it was humbling, difficult, and one of the biggest blessings I’ve ever encountered. (They kept this up for a good 2 weeks after Milkman went back to work after I had the baby. I owe them a very great debt!) My beloved neighbor and dear friend would pop in on the days my family wasn’t here, and she would give me back rubs, and take my kids to water plants and feed chickens to give me little breaks. As someone who is used to being on the go, being a helper, being a host, and taking care of other people, it was totally foreign to be cared for like this, but it was good for me.
One of the big concerns I had after the tear was my ability to deliver this baby vaginally. The pain that I was in had me longing for a C-Section, but! There was an issue that would make a C-Section very undesirable for me. After 7 failed epidurals from my previous labors, and a consult with the head of anesthesia at my hospital, we determined that due to my scoliosis and arthritis, epidurals were never able to be properly placed and take effect. This being the case, it was suggested I try for an epidural at the very beginning of labor (something I’ve never considered), and then if it didn’t take, we would progress to a spinal. If that didn’t work, we would know that if I was in need of a C-section, I would have to go under general anesthesia. The thought of not being the first one to see my baby felt unbearable. Without the ability to move on my own or go anywhere without assistance, I had a lot of time to sit, stew, worry, and cry. And boy, did I cry a LOT!
While some people can fully cook a baby in 37 weeks, I am a slow cooker, and I knew I wouldn’t deliver this baby boy early, let alone “on time”. I normally have weeks upon weeks of prodromal labor, but this time, all prodromal labor stopped at 38 weeks and my uterus was calm and totally disinterested in ejecting a baby. My midwives and my perinatologist knew me well enough to not bother offering an early induction, and we didn’t even try for membrane stripping this time since it had never worked before. We knew the name of the game was “wait”, and so we did.
My sister brought oils, both to diffuse and to slather on me. My neighbor and sister tried pressure points, and Milkman tried making me meals loaded with balsamic and oregano, but nothing could cause my body to kick into gear. This was not surprising given my history, but it was discouraging. From feeling around, one midwife said the baby was really big, and another said the baby was right on track. One ultrasound showed a beast, the other a totally normal sized baby. I felt confident that I could deliver a baby at any size— if only my pelvis weren’t split! But it was split, and I was getting nervous. This was also the first pregnancy where I became terrified of labor. After my last (and very traumatic) birth, I became consumed with terror at the thought of delivering another baby. There were so many moments of Milkman holding me while I gripped his hands to death whispering over and over “I don’t want to do this, I don’t want to do this, I can’t do this, I don’t want to do this…” and him whispering back “you can do this, your body was made to do this, you will do this…” over and over.
I felt like I practically lived at the hospital the last 3 weeks of my pregnancy. Between midwife, perinatologist, and iron infusion appointments to help get my iron up to a safe level for delivery, even the parking garage attendants got to know me. By week 40, the valet was saying “today?” Every time he parked my car and I would say “nope. Not yet.”
At that 40 week appointment, the perinatologist set my induction for 41 weeks, and said hopefully I would go before then. It was at that point that I felt the clock ticking. I was absolutely not interested in an induction, so I figured I would try everything I could at home. We kept up with oils, and I began pumping and nursing around the clock. Sex wasn’t an option because my pelvis was split, but we tried massaging pressure points, and more oregano oil than you can shake a stick at. I went from crying about not wanting to be in labor, to crying and needing to be in labor— but still not wanting to be! That last week of my pregnancy was brutal, and not one I would like to re-live ever again. The pain, the emotional turmoil, the hormones! Just a big mess.
The day before my scheduled induction, I put makeup on, had Milkman push me over to the barn, put heels on me, and shoved my cane under me to prop me up for pictures of my week past date belly pictures. Looking back, I’m so glad we did that! I’m really bad at taking belly pictures when I’m pregnant, so it’s something I’m grateful for!


Sunday morning dawned. The day of my induction was here. Not a contraction or sign of impending labor to be seen. We went to church, and when I came home, we all piled on our bed, while I nursed Peachy, and cuddled my family of 5 for the last time. After lots of tears on my part and the kids’, we loaded them up and took them to my mom’s house. We headed to the hospital, and I told Milkman over and over “I don’t have to stay after they check me, if I don’t want to, right?” And he would say “we can leave any time you want.”
We got to the hospital and got checked into a wheelchair accessible room. I made it clear I wanted to be checked and told if I was favorable for an induction, and if I wasn’t that I would be going home. I was hoping to do a foley and cervadil only to find out that my hospital doesn’t even have cervadil, and I was a 2.5 which meant they wouldn’t do the foley. They said we would go right to Pitocin and because of this, I would not be able to be in the shower (my favorite place to labor) because with pitocin you need constant monitoring. I began crying. How would I make it through a marathon Rachel labor with no shower? I explained how an epidural was not likely to work, and that I wanted to go home and wait for natural labor to start. One nurse was annoyed and said I should just stay, and another nurse went to talk to someone in anesthesia.
I told Milkman to pack my things and though he was supportive, I think he also wanted to just get it over with and begin the induction. At this point I asked a nurse “if I leave now, and come back when I’m in labor, will I be charged twice for being admitted?” She told me I would be charged twice, and being the cheapskate I am, I said “well, I guess I’m staying then”. Soon after then, the nurse came in with a young, female anesthesiologist. She told me that she was looking at my pelvic MRI and x-rays, and she understood why my previous epidurals hadn’t worked, but that after studying them, she was 90% sure she could place a working epidural. Though I had sworn I wouldn’t go through the hassle of getting one that wouldn’t work anyway, I felt really confident in her confidence.
One hour later, I had a working epidural and pitocin running through my veins. 8th time’s the charm apparently!
Because of my disability we had to take several things into consideration and care. One was that I couldn’t open my legs more than about a foot to 18 inches at the knee. Another was that I needed to be moved frequently, but the epidural posed a special threat because I couldn’t feel pain in the same way to trigger me to not move into unsafe positions. I also would not be able to deliver on my back, as it would require my legs to open to far. Because my labors are often very long (34, 23, and 56 hours respectively), being unable to be mobile was a particular concern for extending the length of my induction.
Every 90 minutes, Milkman had an alarm that would go off. He would stabilize my legs with 2 pillows between, tie a sheet around my knees and pillow to keep them closed, and I would move from my right side to my center. 90 Minutes later, we would do the same thing and move from the center to my left side.
9 hours after my induction began, the midwife who delivered Mamitas walked in the room and was officially on duty. We had gotten the schedule a few days before and this was one of the few reasons I decided to stay. Linda is an exceptional midwife. She is the calm to my crazy, she is down to earth, and she can deliver a baby in any position. She is one of those people who radiates warmth, without being syrupy. Real salt of the earth. The team said they were going to check me, and since I had so many contractions they were sure I was close. I told them “pretty sure I’m not.” Guess what? No change. They said maybe a tight 3, but true to my normal, that cervix wasn’t budging. I had a good cry, snuck some food, sipped some of Milkman’s coffee, and told him I wanted to go home. Obviously, it was too late to go home, but this was for the birds. Not used to contracting and not feeling it was totally foreign, so I tried to watch TV, but that made me even more annoyed. I got moved onto my side, Milkman slipped in the bed behind me, and I put in my headphones, turned on my labor mix, pulled my sleep mask over my face, and fell asleep crying silently.
Around 5pm, the Midwife came in and I was about a 5, and the baby was still way up high in my ribs. I told her I was discouraged and she said “I know exactly how this is going to happen. You’re gonna have some crazy contractions and he’s gonna drop, you’re gonna feel pressure and he’s going to engage and be born right after that. This part is taking a while, but once he drops, it’s going to go fast.” I gave a pursed lipped smile and rolled my eyes a little. Nothing ever goes fast for me! We talked about labor positions, and though we had planned on hands and knees, she said “We could tie your legs shut, and if a baby wants to come out, it’ll come out. When the time comes, we’ll get you on your side, nice and comfortable and he’ll make his way out.”
Within an hour, my epidural ran out. I could feel the contractions ramping up, and it felt good to breathe through them. With previous labors, I was so exhausted by the time I hit transition that I would go wild. This time, I moaned low and slow, I breathed deeply, and held onto Milkman like he was a life raft and I was in the middle of a stormy ocean. The pain was satisfying, and because I was well rested, I felt strong enough to handle them. The first song on my labor mix played over and over. A love song…
In April, our foster son left us unexpectedly after just about a year. We were destroyed, and Milkman and I went away on a baby moon. We spent 3 days eating and sleeping (LOTS of sleeping. I took multiple naps a day!) One of the days, Milkman convinced me out of bed long enough to go to the movies and took me to see the movie “A Quiet Place.” If you aren’t familiar with it, the movie is mostly silent. It’s a suspenseful, well acted, beautifully shot thriller, and after watching it, it fast became one of my favorite movies of all time. There was once scene that had me bawling in the theater, and in this scene, John Krasinski And Emily Blunt slow dance with headphones in to the song Harvest Moon by Neil Young. The last 2 months of my pregnancy I would listen to that song, and cry, and hold onto Milkman, feeling a multitude of emotions. Missing our foster baby, being excited to meet our new baby, fearing labor, loving Milkman so much it hurt, ready for the next chapter, but so terribly sad the last chapter had ended. This song became the theme for my unborn baby, and as it played during labor, I would picture being able to stand, and not being so crippled, and swaying with my husband to that dreamy song.
Around 8, my contractions were right on top of each other, I felt a huge turn, and yelped, and boom, he moved down. As it turns out, Midwife Linda knows what she’s talking about. Who’d a thunk? I told Milkman between contractions “Tell… Linda… he’s engaged… coming soon”.

She came in a while later, checked me, and said “well, honey, you’re complete. You start pushing when you want to.” The nurse and Milkman moved me on to my right side, and I felt the urge to push. Linda half laid on the bed, and told me to rest my left knee on her head. My legs were only open that much! I was pushing with all my might, and at one point the baby’s heart rate decelerated, so they threw an oxygen mask on my face. Between pushes, he was going back up. His heart rate went down again, and finally she said “you just gotta push with all your might, and don’t stop” I delivered his head, and I knew he was bigger than my other babies. One contraction later and he was out. It felt longer, but I pushed for less than 10 minutes.

They put him in my arms while he screamed and I opened my eyes wide and said “uh… he’s big, right??” And she replied “oh, he’s BIG!” I nicknamed him Gordito right then and there.
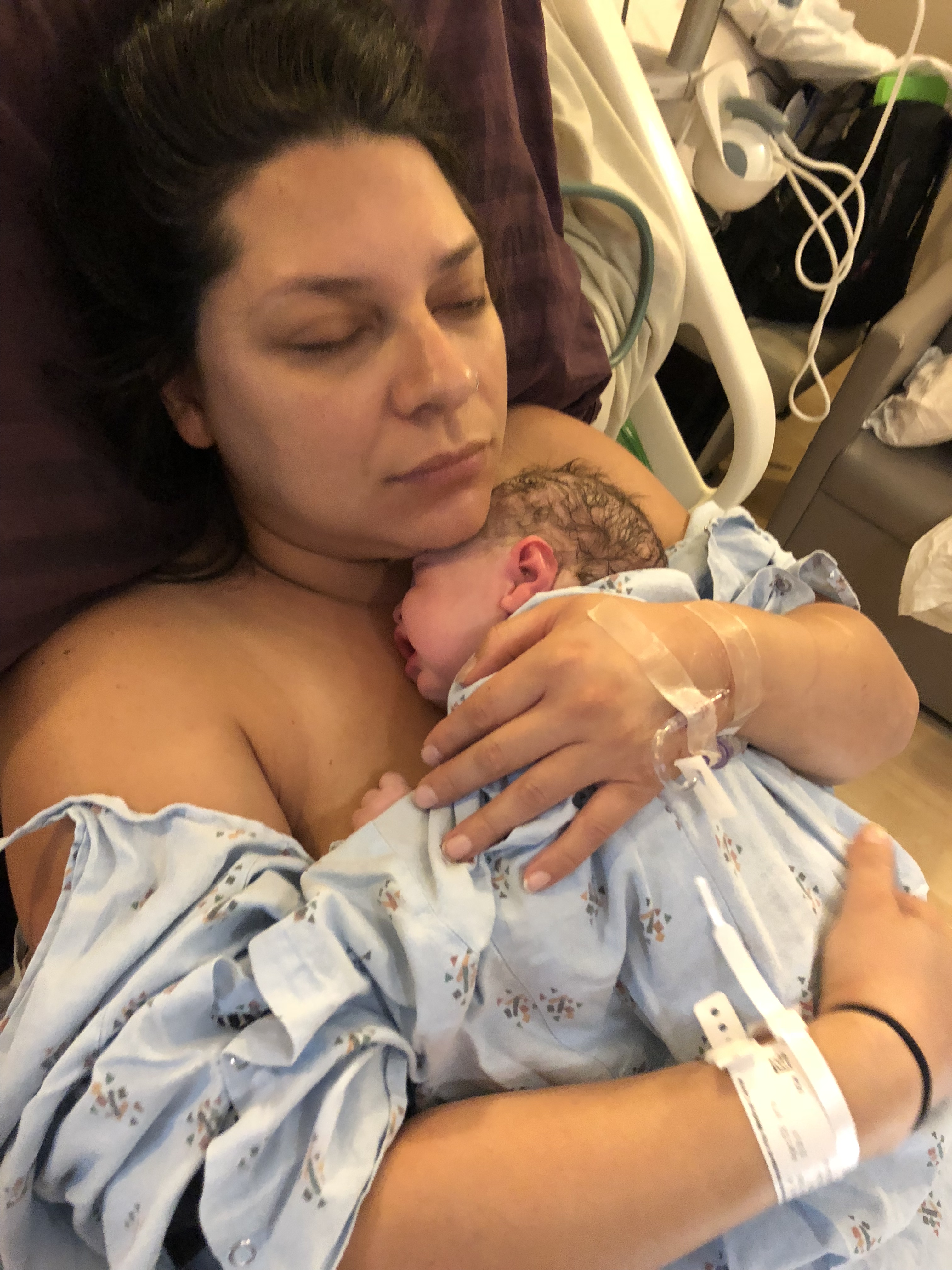
A while later I delivered the placenta. I remember holding the baby and watching Linda look at it curiously. She said it was a huge placenta, she also said it was very mushy, and deteriorating. Praise God I’m such a cheapskate and didn’t want to pay two admitting fees, this baby NEEDED to come out when he did. I have this clear memory of her pushing her finger into it and her finger went clear through the placenta. She called in 2 people to look at it, and she didn’t seem convinced it had all come out. However the doctor inspected it and said it was all there and not to worry.
Milkman and I marveled at our baby. He was so chubby! I checked his lip and tongue almost immediately and saw he was lip and tongue tied, and told Milkman to call the ENT first thing to make an appointment to get it lasered. I was not interested in months of ductal thrush and mastitis like I had with Mamitas, and 24 clogged ducts in 3 months after Peachy! Milkman took a million pictures, I nursed my baby for the first time, which is always super magical, and ate some gluten free graham crackers with peanut butter and drank a pitcher of apple juice (this is what I eat after every single delivery!)

They measured Gordito and he came in at a whopping TEN POUNDS! He was 22 inches long, and a beast. My other babies had been in the 7-8lb range, so giving birth to such a large baby was a shock.
Once everything was removed and I was cleaned up, we were taken to the postpartum wing, and this is where my evening went from a sweet dream to a total nightmare. I began nursing the baby and I felt a very, very large clot pass. The nurses had been “massaging” my uterus post delivery and kept saying it wasn’t feeling right. I hit the call button, my nurse came in and I told her I needed assistance getting to the bathroom as I had passed a large clot. She pulled open my postpartum mesh hospital underwear and her face alarmed me. She said we wouldn’t be going to the bathroom, and that she needed to get the doctor. The charge nurse came in, and within seconds the tiny little room was filled. My midwife was there too. They pulled back the sheet and there was blood everywhere. I was passing massive clots, and I had multiple people pushing on my abdomen while I nursed and switched back to labor breathing. The charge nurse explained the doctor was in a C-section, and they were going to wake the on-call doctor to come in. She was a young, very tall OB, with magnificently long fingers and narrow hands. It was actually one of the first things I noticed about her, which was interesting considering that very soon, I would be introduced to them in a horrifying way. She explained that my uterus wasn’t contracting properly and that I was hemorrhaging. She was going to attempt to sweep my uterus with her hands and pull anything out she could find. She had the nurse crank up some pitocin, and they gave me a shot of morphine. She said “ready?”
I had just delivered a 10lb baby. I could not have understood before that moment how anything could have felt worse than transition and pushing out a 10lb baby, but lo and behold, there is something worse, and it was this. I had a nurse on each side to stabilize my legs and keep them from opening too far and worsening my SP injury, and those long slender fingers, and that thin slender hand went all the way up inside me and she began to scrape and claw at the inside of my raw uterus. It was late, and being in a small postpartum room, I was determined to be quiet so I wouldn’t disturb the sleep of my fellow postpartum mothers and their sweet newborns in the wing, so I contorted and twisted and did Lamaze breathing and moaned as quietly as I could. She pulled out masses of clots and tissue and while I regained my composure she said “there’s more. I’m so sorry, I know this hurts, but I have to try again. You can scream.”
I fought back tears and said “I can’t scream, I don’t want to wake anyone up!” And everyone said “no one would expect anyone to be quiet through this. Just scream.” I handed my newborn to Milkman, and noticed the look of white terror on his face. “Ready?” The OB said. And I yelled out guttural yells and screams while she pulled out yet more tissue and clots. At this point, there was blood dripping off my bed and onto the floor. It was everywhere. I was soaked in it, all the way up my back and down my legs. My husband fought back tears, one of his hands in mine as I squeezed it as hard as I could and the other cradling our newborn baby.
“I can’t get it all out. She has to go in for a D and C.” My heart sank. The one thing I wanted to avoid in this entire birth was going under general anesthesia, and it was going to happen. I nursed the baby while they waited for the other doc to get out of the C-Section. I remember looking at the floor as I handed the baby off to Milkman and kissed them both, and being shocked at the amount of blood in the room. If it hadn’t been for those iron infusions leading up to the birth, I may not have survived.
The team that took over in Pre-Op was a nightmare. While I was somewhat comfortable with the OB in charge, as he had delivered my oldest, the nurses and the anesthesiologist were like vinegar to the teeth. I was tired, it was the middle of the night, I had delivered a baby, and experienced some of the worst pain in my life. The nurses were mouthy and the anesthesiologist was cocky. I had the OB who was going to do the surgery do an internal ultrasound before I went under to confirm that the procedure was necessary. I remember looking at the screen on the machine and it looked like my uterus was full of cotton. He confirmed we had to do it, and we had to do it now. I cried and the nurse said “you don’t want to do this? You could lose your uterus, or you can lose your life! Is that what you want? You literally could die right now.”
I said “I know I need it, but I’m sad because my brand new baby is down the hall and I’m going into surgery!” She said I needed to calm down. I wanted to drop kick her, but I held my tears back. The last thing I remember is the doctor telling me “how far can we open your legs?” I showed him, he measured, and he had every person in the room look and said “don’t open her legs past this point. We don’t need her in a wheelchair for life.” Then the anesthesiologist strapped my arms down, and they said “see you in 45 minutes”, and I was out.
I woke up crying, which is typical for me coming out of general. I asked what time it was, and they told me it was 3 hours later. Apparently they still couldn’t stop the bleeding, so they tried putting a foley inside my uterus and inflating it to put pressure to assist in stopping the hemorrhage. Unfortunately, they couldn’t keep the foley in because my cervix also wasn’t going back down. To this day, I’m not totally sure what went down in that operating room, but all I remember is the doctor telling me “it didn’t go according to plan, but we saved your uterus.” I asked the nurse to take me to my baby, and she refused. I told her I needed to breastfeed my baby and she said “you need to rest!” I said I could nurse and then rest, but I needed to see my baby. She threatened me again with losing my uterus or my life, so I asked to talk to my husband. Later he told me that she told him “you need to be on my side, don’t tell her she needs to come back.”
I told him they weren’t letting me come back to the room and that he needed to call my sister, it was now 5am, and tell her to come to the hospital and nurse the baby. He spoke to the nurse and said “I know it isn’t visiting hours, but I’m going to have my sister in law come nurse the baby since they aren’t releasing Rachel.” The nurse looked shocked at the thought of someone else coming in to nurse the baby and then made a call or two, and magically I was released back to my room!
Milkman looked totally wiped by the time I came back. He was holding out sweet little fatlng and got choked up when he saw me. He kissed me over and over and said he was terrified that he was going to lose me forever that night. I latched my sweet newborn on, and nursed him, Milkman crawled into the bed next to me, and we slept, very much alive, and very blessed to be together.
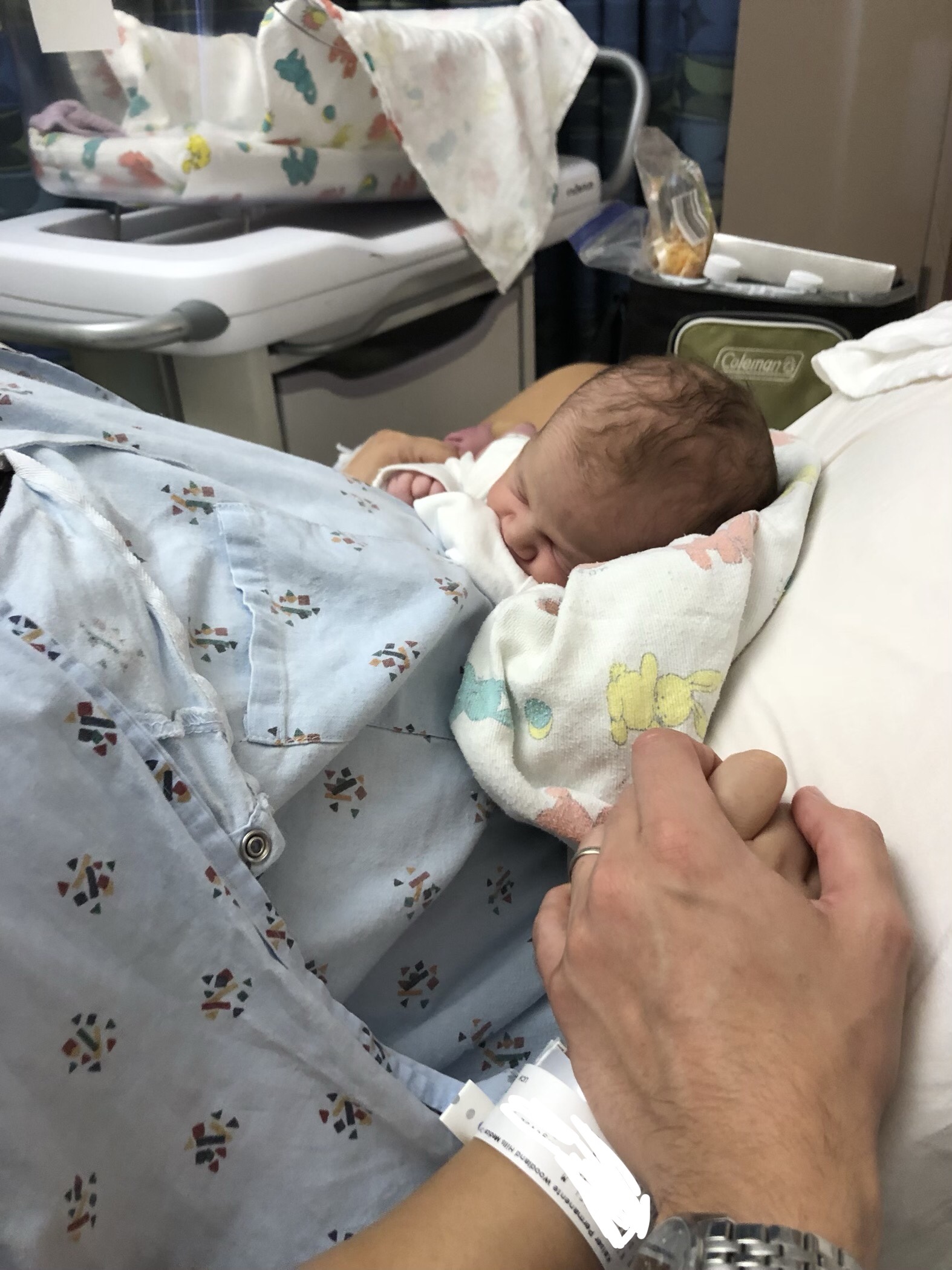
———
I never know where to stop these birth stories. There was a lot more that happened before, during, and after, but this was so long as it was. I was encouraged by my besties not to worry about the length of the story, because at the end of the day, I’m writing this story for Gordito and for me. I want to remember these things, and I want him to know how he entered this world.
It’s strange to me that his labor was my shortest at just 18 hours, and that while he was my biggest, he was my easiest delivery. The aftermath was terrible, his size likely played a part in my hemorrhage, but I am so glad that things ended as favorable as they could have!
This was also the first time postpartum that I felt the docs realized the severity of my disability. The day after delivery, they had a pelvic floor therapist in my room assessing me, and put in a referral for me to receive pelvic floor therapy when I got home. It took 9 months of weekly appointments to get me out of the chair, off the walker, and only needing my cane for flare ups or long walks. I’m so grateful for the care I received postpartum. I also had a bunch of iron infusions after delivering, and was well cared for in that respect.
A year out and Milkman still gets choked up thinking about the hemorrhage. In some ways, I feel like that wasn’t even me, but I am grateful to be alive!
My baby is one today. He is the love of my mama life, he’s my little (BIG) best friend. At a year, he loves to babble, laugh, be tickled, and make funny noises. He’s a very anti-social baby and only has eyes for mama and papa— but especially mama. We never get to be alone or go on a date because he can’t handle being apart from me, but I’ll tell you, it’s worth him tagging along, because even when I’m most burnt out, I look at his chubby face, ridiculous toothy grin, and he snuggles into the crook of my neck, signs to nurse, and I’m smitten all over again.
Happy 1st Birthday, my sweet baby boy.



































